Abstract: HIV infections including AIDS have now become an almost developmental and security problem in most developing countries, in addition to its medical, social and economic consequences affecting the individual, home, society and country. AIDS, first reported in women in 1981, is a major concern for women and girls affecting their motherhood also. Globally, to date 48% of people living with HIV are women and this rate is gradually going up Biologically women are more susceptible to get the infection, even though not much difference is seen in the progression of the disease.
Keywords: HIV infections prevention, AIDS, adult HIV prevalence, STDs/STIs prevention programmes, sexual partners
Introduction:
HIV infections including AIDS are one of the pandemics affecting the world in the 21st century. It had its origin in early 1980’s. No other disease has gained so much “popularity” within this short period. It is even threatening the security of countries especially the underdeveloped and developing ones which have more than 95 % of this infective disease. It is worth quoting here the words of Peter Piot, Executive Director of the Joint United Nations Programme on HIV /AIDS (UNAIDS),“ We do not have a cure; we do not have a vaccine. The primary strategy to reduce the spread of HIV is behavior change. And it is much harder to change an adult’s behavior than it is to help young people adopt safer behavior from the very start of their sexual lives”. The UN secretary general has called the HIV /AIDS epidemic “The most formidable development challenge of our time which needs a global commitment for intensified and coordinated action”. “You can’t get AIDS by kissing, hugging or holding hands. We are normal human beings. We can walk, we can talk, we are all the same. When I have an open wound, that is the only time people need to be afraid of me”. These are the words of the 11 year old Nkosi Johnson at the opening ceremony of the International AIDS Conference in the city of Durban in the year 2000. This was the poor young South African boy who got infected at birth. What he said is true also.
Even though much awareness has occurred in this field , the problem of HIV /AIDS is growing in magnitude worldwide and the cost in human life and suffering is staggering. HIV /AIDS which was regarded primarily as a serious health crisis, a decade ago, is now clearly a development crisis and in some parts of the world is becoming a security crisis too. This will have a profound impact on infant, child and maternal mortalities , life expectancy and economic growth. Raising public awareness on change in moral behavior is the key factor in prevention programmes. HIV / AIDS epidemic affects and kills people in their more productive years ( 20-45 yrs ). HIV infection leads to increased morbidity and mortality in their most reproductive ages and it will have serious economic consequences on the family, the community and the nation. There will be a drop in life expectancy and a loss of skilled forces across all levels. The catastrophe of HIV /AIDS can undermine the achievements we have gained in the health field, like increase in life expectancy, decrease in infant and maternal mortality rates etc. Even the 4 million people currently living with HIV /AIDS in India will be in an extra burden on the already over stretched health care system.
The AIDS epidemic has a profound impact on growth, income and poverty. It is estimated that the annual per capita growth in half the countries of sub-Saharan Africa is falling by 0.5– 1.2% as a direct result of AIDS. By 2010, per capita GDP in some of the hardest hit countries may drop by 8% and per capita consumption may fall even farther. Calculations show that heavily affected countries could lose more than 20% of GDP by 2020. People at all income levels are vulnerable to the economic impact of HIV/AIDS, but the poor suffer most acutely. One quarter of households in Botswana, where adult HIV prevalence is over 35%, can expect to lose an income earner within the next 10 years. A rapid increase in the number of very poor and destitute families is anticipated. Per capita household income for the poorest quarter of households is expected to fall by 13%, while every income earner in this category can expect to take on four more dependents as a result of HIV/AIDS. In the worst affected countries, steep drops in life expectancies are beginning to occur, most drastically in sub-Saharan Africa, where four countries (Botswana, Malawi, Mozambique and Swaziland) now have a life expectancy of less than 40 years. Were it not for HIV/AIDS, average life expectancy in sub-Saharan Africa would be approximately 62 years. In South Africa, it is estimated that average life expectancy is only 47 years, instead of 66, if AIDS were not a factor (see Figure 2). And, in Haiti, it has dropped to 53 years as opposed to 59. The number of African children who had lost their mother or both parents to the epidemic by the end of 2000— 12.1 million— is forecast to more than double over the next decade. These orphans are especially vulnerable to the epidemic, and the impoverishment and precariousness it brings. As more infants are born HIV-positive in badly affected countries, child mortality rates are also rising. Unequal access to affordable treatment and adequate health services are some of the main factors accounting for drastically different survival rates among those living with HIV/AIDS in rich and poor countries and communities. This holds good for our country also.
What is HIV / AIDS ?
The Human Immunodeficiency Virus (HIV ) causes a chronic infection that leads to profound immunosuppression. The course of the infection may vary somewhat, with some individuals developing immunosuppression within 2-3yrs and others remaining free of immunosuppression for 10-15 yrs. Eventually the infected individual develops early symptomatic HIV, which progresses to AIDS.AIDS is the acronym for Acquired Immune Deficiency Syndrome which forms one fatal end stage in the natural progression of HIV infection. HIV infection means any individual harbouring the organism, who may or may not have any disease manifestation,which includes AIDS also. But at the same time they can transmit the infection to others in certain peculiar circumstances which we will discuss later. So the outward appearance of an individual need not tell us whether he is harbouring the virus or not. After acquiring the virus, the mean duration by which it progress to AIDS is 10 yrs.
Origin of the Disease:
The medical community was surprised in the early 1980’s, by reports of a particular type of pneumonia caused by Pneumocystis carini in 5 otherwise healthy young men from Los Angeles between October 1980 and May 1981 and a series of other 26 cases of a particular skin cancer called Kaposi’s sarcoma, again in healthy young men. Prior to these reports these diseases were seen in elderly persons with immunosuppression and that also equally in males and females. Further it was found that all these young otherwise healthy were homosexuals, thus attributing something related to sexual activity as the cause. Later it was also detected in those who received blood transfusions, and in intravenous drug abusers (IVDU). Research work later identified a peculiar type of virus belonging to the group of retroviruses as the cause by Montagnier and Galo. In 1983 the virus was isolated from a patient with lymph node enlargement. In 1984 it was confirmed to be the cause of AIDS.
When and how the disease originated is controversial. Retrospective analysis done on stored blood showed that the earliest case identified dates back to 1959. Even though various theories of origin of the disease are there, the most reliable is that the virus was present in certain chimpanzees in Africa ( Pan troglodytus troglodytus ) from ancient times without producing disease in them but getting transmitted among them from generation to generation – leading to mutations making them pathogenic. In certain African forest areas these animals were slaughtered for food purpose and, by injuries in hand the organism might have entered the human being and from that individual to his sexual partner. When both of them die the virus also gets arrested there. But due to the behavioral pattern of man in the latter half of 20th century, with much travel for education and job and due to increasing promiscuous sexual behavior, the virus might have spread first among homosexuals and gradually to bisexuals. The virus might have moved from forest to cities. Now it has become a heterosexual disease causing concern for all groups of individuals irrespective of age or sex or race. So it is the behavior of the human population which paved the way for its spread. In New York, in the Stonewall Inn , by the gay revolution it spread among homosexuals. So initially it was thought that homosexuals are more affected by the disease. Now it is seen equally in homo and heterosexuals world-wide, but in the US even now the main mode of transmission is homosexual contact and intravenous drug abuse (IVDU).
Virus and the Disease:
HIV is a retro virus belonging to lentivirus family and is icosahedral in shape. It consists of RNA and a peculiar enzyme called reverse transcriptase. This is covered by an inner protein and an outer lipoprotein membranes, in which are seen the important antigenic determinants — gp-120 and gp –41 in the outer cover and p18 & p24 in the inner cover. There are two types of HIV i.e. HIV –1 & HIV –2. HIV –1 is more common in the US. After it enters human body ,the ideal site in which it likes to reside, host cell is a peculiar type of lymphocytes, one type of white blood cells, called CD 4 T cells with CD 4 molecule on its surface. These lymphocytes are important in preventing infections and in immune surveillance and tumor prevention normally. This primary infection occurs by entry of organism through sexual / other routes. Gradually the virus increases in number in the body and leads to an “ acute HIV syndrome” simulating a viral fever. In this stage the patient is highly infectious because of high levels of virus in blood, but at the same time the disease cannot be detected by blood tests. Then gradually immune response occurs against the virus and the virus gets trapped in lymph nodes and viremia and the acute symptoms stop and patient goes into a latency stage, on the average of 10yrs. Gradually, the metabolism of the virus inside these cells leads to progressive quantitative and qualitative deficiency of CD 4 cells. Then slowly CD4 cells decrease and when it reaches a particular level the patient develops various infections and cancers. Initially these may not be life threatening, but when the CD4 count drops to very low levels, the patient develops serious infections and malignancies and succumbs to that. This fatal stage is called AIDS. Even though various groups of drugs are there to decrease viral multiplication, drug treatment is costly and is with various side effects, needing constant supervision of a specialist.
Transmission:
The main modes of transmission of HIV are:
1. Sexual contact – homosexual, heterosexual &bisexual
2. Blood & blood products transfusion and organ transplantation
3. Intravenous injections and drug abuse
4. Mother to foetus
5. Occupational exposure
More than 80 % of HIV cases are transmitted by sexual contact. Intimate body contact during the sexual act leads to minute abrasions and injuries in the skin and mucosa. Through these injuries the body fluids of one partner can enter the other and the virus can enter the body. Semen and vaginal fluids contain plenty of organisms. Also if there is an ulcer in the genitalia or urethral discharge the chance for transmission of the infection increases. That is why the presence of other sexually transmitted infections as syphilis, herpes genitalis and gonorrhea is said to increase the chance of transmission. Through vaginal mucosa it can be transmitted especially if traumatized. So there is 20 times more chance of HIV transmission from man to woman than from woman to man by vaginal intercourse. This is because in females there is increased exposure of vaginal and cervical mucosa as well as endometrium of uterus to infected semen. In males the penis and urethral orifice are exposed only to a brief period to the infected vaginal fluid. Persistent and proper use of condoms can significantly reduce this mode of transmission. In receptive anal intercourse due to increased trauma and due to some other reasons the chance of transmission is increased more than that by vaginal intercourse. Vaginal mucosa is several layers thicker than rectal mucosa. The chance of transmission by oral sex is less but the disease can occur and cases have been reported. Behaviors that bring the highest risk of infection in Asia and the Pacific are unprotected sex between clients and sex workers, needle sharing and unprotected sex between homosexual men. But infections do not remain confined to those with higher-risk behaviour. Many countries have seen major epidemics grow out of initially relatively contained rates of infection in these populations. Northern Thailand’s epidemic in the late 1980s and early 1990s was primed in this way. Over 10% of young men became infected before strong national and local prevention efforts, including the ‘100% condom programme’, reduced high-risk behaviour, encouraged safer sex and lowered HIV prevalence. Few countries are acting vigorously enough to protect sex workers and clients from the HIV virus. Yet, it is from the comparatively small pool of sex workers first infected by their clients that HIV steadily enters the larger pool of still-uninfected clients who eventually transmit the virus to their wives and partners. Although recent behaviour surveillance surveys show that in 11 out of 15 Asian countries and Indian states, over two-thirds of sex workers report using a condom with their last client, the need to boost condom use remains. In Bangladesh, Indonesia, Nepal and the Philippines, for instance, fewer than half of sex workers report using condoms with every client.
The best way to prevent transmission by sexual means is to follow certain principles in life. These are – never have sex before marriage and be faithful to the spouse after marriage. These should be stressed especially in early adolescence i.e. before starting any sexual activity. It is seen that sexual activity before marriage is more common and begins more early in boys. i.e., between the ages of 10 and 15. If one cannot follow these things, advise about safer sex, as proper and consistent use of condoms. Also try to avoid contact with promiscuous individuals, commercial sex workers and unknown persons. Semen during artificial insemination can also transmit infection.
Blood and blood product transfusions and organ transplants, if infected, can transmit the disease by direct entry of organism into the body. The chance of transmission by transfusion of one bottle of infected blood is nearly 90 100%. The chance of transmission by an unprotected sexual contact from an infected individual is 1in 1000. But more than 80 % of HIV cases are sexually transmitted. Blood transfusions leading to transmission are becoming rare because of proper screening of blood before transfusions. Also blood from high risk individuals should be avoided. Intravenous injections using infected syringes and needles also can transmit the infection. Government has put forward various directions to prevent these modes of transmission. By using properly sterilized glass syringes and needles, cleaned and sterilized in boiling water for 30 minutes or by using reliably new disposable syringes and needles this can be averted. HIV virus can be killed by one minute boiling, but Hepatitis organism is killed only by 10 minutes and various spores can be killed only by 20 –30 minutes boiling. The disease can also be spread through the skin or mucosa of an individual coming in contact with infected material from another individual as blood, semen, vaginal secretions, other body fluids as urine, feces etc contaminated with blood. Even though the organism won’t enter through intact skin or mucosa, care should be taken to handle these materials because minute injuries in the skin or mucosa are usually not visible to naked eye. Usually tears are noninfectious, but in the case of saliva it is controversial. So proper care should be taken, as using gloves, in handling open wounds in any situation. Also it is advisable, as far as possible, not to come in direct skin contact with anybody secretions or excretions of another individual.
Using of improperly sterilised needles and syringes or sharing of these equipments among intravenous drug abusers is another important cause of transmission. Sharing injecting equipments is a very efficient way of spreading HIV, making prevention programmes among injecting drug user populations another top priority. Upwards of 50% of injecting drug users have acquired the virus in Manipur in India, Myanmar, Nepal, Thailand and China’s Yunnan Province. Extensive harm reduction programmes can and do work. By the late 1980s, Australia had prevented a major epidemic from occurring among injecting drug users and, quite likely, from spreading beyond them. Such examples are being followed by several other countries but in an isolated fashion. The SHAKTI Project in Dhaka, Bangladesh, offers injecting drug users needle exchange, safer injecting options and safer sex education, as well as condoms.
Transmission of the infection from mother to the child can occur in the utero, more commonly during vaginal delivery due to trauma in vagina and coming in contact with cervical and vaginal secretions, and after delivery. The chance of materno fetal transmission is 20 –30 % for each pregnancy. Breast feeding by an infected mother can transmit the disease to a baby through breast milk, if it is already not infected. So in developed countries they advise an infected mother not to breast feed and to give completely artificial feeding. But in developing countries like India where artificial feeding is not feasible always, and improper feeds can lead to malnutrition and progression of AIDS more rapidly in the child, this is debatable. Another point to remember is that a pregnant lady if HIV positive has to take drugs which decrease transmission of the virus to the fetus, under supervision. Most often such a child will invariably become an orphan within a few years because the father and mother might be infected in such cases.
To our knowledge till now, HIV is not transmitted by casual body contact as shaking hands or by insect bites or mosquito bites.
High Risk Groups :
The following are the high risk individuals in society who should be monitored.
- Patients with other sexually transmitted disease as syphilis, herpes genitalis, gonorrhoea which can produce genital ulcers /or urethral symptoms
- Individuals in the high risk category – Intravenous drug abusers, homosexual and bisexual males, those undergoing regular blood transfusions, regular sexual partners of such high risk individuals, sexual partners of a known HIV patient, commercial sex workers and their sexual partners, heterosexual persons with multiple sexual partners or unprotected intercourse.
- Persons who consider themselves at risk.
- Health care workers who perform invasive procedures Donors of blood, semen and organ.
- History of transfusion after 1985 of unscreened blood or blood products. It is advisable to screen these individuals.
How to detect HIV infection ?
1. Enzyme Linked Immuno Sorbent Assays – the commonly called ELISA test – are widely used to screen the presence of HIV infection. In this the test detects presence of antibodies in the blood of a patient harbouring HIV. This is important because clinically the patient may not have any symptoms/signs to diagnose HIV and so the infection goes unnoticed . But such an individual can spread the infection in certain particular risk behaviors as discussed above .But in the initial 3-4 weeks of infection it may not produce a positive result because for development of HIV specific antibodies, it takes about 3-4 weeks after acute infection. Also conditions other than HIV infections can lead to a false positive result. So any individual who is undergoing an ELISA check up for HIV is advised to have a pretest and post test counselling by a trained counsellor. In the pretest counselling patients should be made aware of the ‘ window period ‘ for the HIV test – that a period of 12 weeks since the last possible exposure to HIV should have elapsed by the time of the test or otherwise it may be a false negative one.
2. Western Blot tests : This is used to confirm an ELISA reactive serum as a true positive or not. It detects antibodies and the specific HIV proteins against which it is directed. It also may not be positive in the initial 3 to 4 weeks of infection.
3. Other tests which can be done include: antigen detection ( p24 assays), CD4 counts to assay the level of immunosuppression to decide on treatment and Polymerase Chain Reaction (PCR ) for measuring the amount of viral particles and rarely viral culture.
Manifestations :
Most often an individual harbouring the virus doesn’t have any initial manifestations and go on transmitting the disease under the high risk behavior states previously discussed, if proper protective measures are not taken. Only years after acquiring the infection, a majority will show symptoms and will be diagnosed. After a prolonged period of asymptomatic stage the patient develops various infections and malignancies and finally AIDS. The important symptoms include loss of 10 % body weight, chronic diarrhea of one month duration, some types of tuberculosis, a ‘thrush ‘like fungal infection in the oral cavity and oesophagus, certain neurologic manifestations and some peculiar types of skin diseases.
Burden of the Problem :
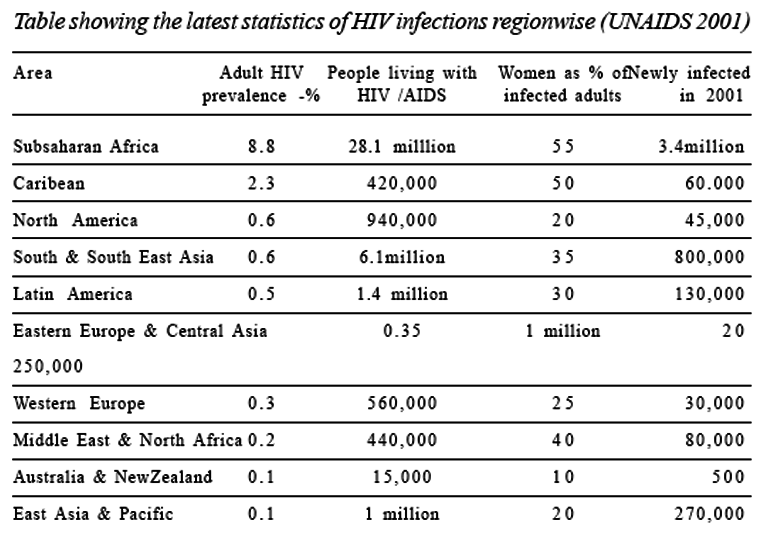
Global burden : Twenty years after the first clinical evidence of acquired immuno deficiency syndrome was reported, AIDS has become the most devastating disease mankind has ever faced. Since the epidemic began, more than 60 million people have been infected with the virus. HIV/AIDS is now the leading cause of death in sub-Saharan Africa. Worldwide, it is the fourth-biggest killer. The diversity of HIV’s spread worldwide is striking. But in many regions of the world, the HIV/AIDS epidemic is still in its early stages. While 16 sub Saharan African countries reported overall adult HIV prevalence of more than 10% by the end of 1999, there remained 119 countries of the world where adult HIV prevalence was less than 1%.UNAIDS latest statistics shows that globally 40 million adults and children were living with HIV / AIDS at the end of 2001. Of infected adults, 48 % were women. In 2001, the global adult HIV prevalence rate was 1.2 %. During 2001, 5 million people were newly infected. There were 3 million adult and child deaths due to HIV /AIDs in 2001. Since the beginning of the epidemic, there have been 25 million AIDS deaths.
The Sub- Saharan Africa has the maximum number of HIV positives 28.1 million with a percentage prevalence of 8.8 in adults. In this area 55% of infected adults are women. HIV prevalence rates have risen to alarming levels in parts of southern Africa, where the most recent antenatal clinic data reveal levels of more than 30% in several areas. In Swaziland, HIV prevalence among pregnant women attending antenatal clinics in 2000 ranged from 32.2% in urban areas to 34.5% in rural areas; in Botswana, the corresponding figures were 43.9% and 35.5%. In South Africa’s KwaZulu-Natal Province, the figure stood at 36.2% in 2000. This notwithstanding, in some of the most heavily affected countries there is growing evidence that prevention efforts are bearing fruit. One new study in Zambia shows urban men and women reporting less sexual activity, fewer multiple partners and more consistent use of condoms. This is in line with earlier indications that HIV prevalence is declining among urban residents in Zambia, especially among young women aged 15– 24. Progress is also being made on the treatment and care front. In the southern African region, relatively prosperous Botswana has become the first country to begin providing antiretroviral drugs through its public health system, thanks to a bigger health budget and drug price reductions negotiated with pharmaceutical companies.
In Australia, Canada, the United States of America and countries of Western Europe, a pronounced rise in unsafe sex is triggering higher rates of sexually transmitted infections and, in some cases, higher levels of HIV incidence among men who have sex with men. The prospect of rebounding HIV/AIDS epidemics looms as a result of widespread public complacency and stalled, sometimes inappropriate, prevention efforts that do not reflect changes in the epidemic. In Japan, meanwhile, HIV infections are also on the rise.
The rise in new HIV infections among men who have sex with men is striking. In Vancouver, Canada, HIV incidence among young men who have sex with men rose from an average of 0.6% in 1995– 1999 to 3.7% in 2000. In London, reported HIV infections among gay men are also on the rise. Rising incidence of other sexually transmitted infections among men who have sex with men in places like London confirms that more widespread risk-taking is eclipsing the safer-sex ethic promoted so effectively for much of the 1980s and 1990s. Similar trends are being detected among the heterosexual populations of some countries, especially among young people. Diagnoses of gonorrhoea and syphilis among men and women have hit their highest levels for 13 years in England and Wales, for instance. But in high income countries since 1996 the life saving anteretroviral drugs which are costly are in use. Deaths attributed to HIV in the USA, for instance, fell by a remarkable 42% in 1996– 97, since when the decline has levelled off.
However, this wide access to antiretroviral therapy has encouraged misperceptions that there is now a cure for AIDS and that unprotected sex poses a less daunting risk. High-risk behaviour is increasing, as a result. In high- income countries there is evidence that HIV is moving into poorer and more deprived communities, with women at particular risk of infection. Young adults belonging to ethnic minorities, including men who have sex with men, face considerably greater risks of infection than they did five years ago in the USA. African-Americans, for instance, make up only 12% of the population of the USA, but constituted 47% of AIDS cases reported in 2000. As elsewhere in the world, young disadvantaged women, especially African-American and Hispanic women, in the USA are being infected with HIV at higher rates and at younger ages than their male counterparts. In USA, sex among males is still the main mode of transmission accounting for some 53% of new HIV infections in 2000. But almost one-third of new HIV-positive diagnoses were among women in 2000. In this latter group, an overlap of injecting drug use and heterosexual intercourse appears to be driving the epidemic. Indeed, injecting drug use has become a more prominent route of HIV infection in the USA, where an estimated 30% of new reported AIDS cases are related to this mode of transmission. In Canada, women now represent 24% of new HIV infections, compared to 8.5% in 1995.
The HIV epidemic in western and central Europe is the result of a multitude of epidemics that differ in terms of their timing, their scale and the population they affect. Portugal faces a serious epidemic among injecting drug users. Of the 3733 new HIV infections reported there in 2000, more than half were caused by injecting drugs and just under a third occurred via heterosexual intercourse. Reports of new HIV infections also indicate that sex between men is an important transmission route in several countries, including Germany, Greece and the United Kingdom. Unfortunately, HIV reporting data are uneven in several of the more affected countries, including some of those believed to be most affected by the epidemic among injecting drug users. In Japan, Germany and United Kingdom, the number of HIV infections detected in men who have sex with men has risen sharply in recent years, with male-male sex now accounting for more than twice as many infections in men as heterosexual sex. This is a major departure from past patterns: until two years ago, the number of new infections reported in both groups was roughly equal. Eastern Europe— especially the Russian Federation— continues to experience the fastest-growing epidemic in the world, with the number of new HIV infections rising steeply with increase in other sexually transmitted diseases and increased rate of IV drug abuse.
 |
Developing Countries :
More than 95 % HIV infections are now in the developing countries. In many parts of the developing world, the majority of new infections occur in young adults, with young women especially vulnerable. About one-third of those currently living with HIV/AIDS are aged 15– 24. Most of them do not know they carry the virus. Many millions more know nothing or too little about HIV to protect themselves against it. In Asia and the Pacific, an estimated 7.1 million people are now living with HIV/AIDS. The epidemic claimed the lives of 435,000 people in this region in 2001. The apparently low national prevalence rates in many countries in this region are dangerously deceptive. They hide localized epidemics in different areas, including some of the world’s most populous countries. There is a serious threat of major, generalized epidemics. But, Cambodia and Thailand have shown that prompt, large-scale prevention programmes can hold the epidemic at bay. In Cambodia, concerted efforts, driven by strong political leadership and public commitment, lowered HIV prevalence among pregnant women to 2.3% at the end of 2000— down by almost a third from 1997.
In Asia & India :
The heavily populated countries in the world such as India, China and Indonesia registered a marked increase in HIV cases, even though HIV/AIDS had a late arrival to Asia. Until the late 1980s, no country in the region had experienced a major epidemic. This situation is now rapidly changing. In 2001, 1.07 million adults and children were newly infected with HIV in Asia and the Pacific. At the end of 2000, the national adult HIV prevalence rate in India was under 1%, yet this meant that an estimated 3.86 million Indians were living with HIV/AIDS— more than in any other country besides South Africa. Indeed, median HIV prevalence among women attending antenatal clinics was higher than 2% in Andhra Pradesh and exceeded 1% in five other states– Karnataka, Maharashtra, Manipur, Nagaland and Tamil Nadu– and in several major cities including Bangalore, Chennai, Hyderabad and Mumbai. India’s epidemic is also strikingly diverse, both among and within states.
In India with more than 1 billion population, national prevalence loses its meaning. In India it is in the rising or trajectory stage with many case hidden under the iceberg with the estimated ones forming only a part of the cases. India has several HIV epidemics with different patterns and prevalence. The epidemics vary significantly from state to state. Heterosexual transmission is more in Maharashtra and Tamil Nadu, whereas those associated with injecting drug use is most common in Manipur. In general, there is a comparatively high HIV prevalence in western and southern India and low in the eastern and northern parts. This heterogeneity together with big differences in social structures and the enormous size and population of India, make it difficult to monitor the various epidemics and institute effective interventions. This has probably contributed to the rapid and continuing spread of HIV in India despite the ten year grace period India experienced from the start of the epidemic in western countries and in Africa in the early 80’s until the prevalence rose abruptly in India. The Indian states of Maharashtra, Andhra Pradesh and Tamil Nadu, each with at least 55 million inhabitants, have registered HIV prevalence rates of over 2% among pregnant women in one or two sentinel sites and over 10% among sexually transmitted infection patients— rates far higher than the national average of less than 1%. In the absence of vigorous prevention efforts, there is considerable scope for further HIV spread. Even HIV prevalence rates as low as 1% or 2% across Asia and the Pacific, which is home to about 60% of the world’s population, would cause the number of people living with HIV/AIDS to soar.
Kerala:
In India due to the diversity in social and cultural factors the state of HIV also differs. States as Arunachal Pradesh has reported almost no HIV infection, and in general other states have reached an adult HIV prevalence rates of 2% or more. In most of our states and in Kerala often it is seen that the infection in females including pregnant women is from husbands who had been infected in turn by sex workers, and these are more in those who travel much for job purposes. NACO estimates that in Kerala 70,000 to 1 lakh people are living with HIV. Patients having an STD has 10 % more risk. In Maharashtra, Karnataka, Andhra Pradesh, Tamil Nadu & Manipur the antenatal rate is greater than 1 %. In Kerala , in antenatals the rate is less than 0.2%, but in STD cases it is greater than 5%. In Kerala most of the cases are from outside, because at least in 40 % of families in kerala atleast one member is living outside. The other peculiarities seen are that most often ladies get infection from their husbands and the male female ratio is 3:1. In other parts of India it is more seen in urban places but in Kerala it is prevalent equally in urban and rural areas.
In India 50 % of the cases are seen in those less than 25 yrs of age but in Kerala infection in those aged less than 25 yrs is less. More than 70% of HIV infections world-wide are estimated to result from sex between men and women. Nearly 80% of cases in India and 95% of cases in Kerala are reported to be caused by heterosexual transmission. According to sentinel surveillance Kerala comes in group 3 in which HIV infection in any of the high risk groups is still less than5% and less than 1% in antenatal women. Now HIV infection is percolating from very high risk to low risk groups.In the Indian context due to varied cultural characteristics, traditions and values with special reference to sex related risk behaviour, infection shifts from high risk population to general population over a period of time.
HIV and Women :
HIV affects both women and men. AIDS was first reported in women in1981. World-wide, more men are living with AIDS, but women are contracting HIVat a faster rate. Women are biologically more vulnerable to transmission. Of the total 40 million affected in the world,48 % are now women. Women are more susceptible to HIV because of the behaviour of men especially in sexual life . On the average, men have more sex partners than women either male or female and so more opportunity to contract and transmit the diseases. Also men have more influence over whether or not to have safer sex. Gender inequalities are important. In most societies women have less access to health care, education and employment. Their unequal situation is reinforced in many societies by the double standards of sexual morality. When women are subjected to violence or sexual abuse, it is conveniently said that women ‘get what they deserve.’ In certain societies the double stand is that women are expected to preserve their virginity until marriage, but young men, on the other hand , are encouraged to gain sexual experience and indeed having many sexual relationships may make a man popular in the eyes of his peers. In some societies having sex with a young girl is believed to increase virility and is seen as a risk minimization strategy by older men or is thought to cure HIV. Yet older, sexually active men are more likely to be HIV infected. While trying to decrease their risk of ‘becoming HIV infected, they are in fact putting young girls at risk of HIV, other sexually transmitted diseases and unwanted pregnancies. Many women who test positive for HIV face the twin prospects of coping with their diagnosis and finding a way of informing their husbands or male partner. In such situations men and their family members may accuse the woman of bringing HIV into the house hold – even though it is much more likely that the man is responsible. In extreme cases, women with HIV may be ejected from their home by their husbands or by the husband’s family after his death. Now the male female ratio is nearly becoming equal with a rapid increase in female cases. An estimated 13.2 million children have been orphaned due to AIDS till now.
Gender Issues in HIV /AIDS :
1. Male violence against women – In most societies there is a double standard of sexual morality, which ensures that women can be viewed as creatures that lead men ‘astray ’. Sometimes, dressing and appearing attractive suffices to earn a woman the label of ‘sexual promiscuousness’. When women are subjected to violence or sexual abuse, it is conveniently said that women ‘ get what they deserve ’.
2. Women’s economic dependency on men – In many societies women have less access to health care, education and employment. Women are also likely to have less formal education, less knowledge of HIV, language barriers and financial issues. In most societies they are dependent on males economically and socially, in their health seeking behaviour.
3. Ideologies of motherhood. In most parts of India especially North India and other developing countries, early pregnancy and delivery are very common, at an age in which the girl is not mentally and physically prepared for motherhood
4. Traditional norms which make it difficult for women to seek treatment and information about sex –In many societies, cultural barriers can inhibit public discussions of sexuality and therefore prevent a better understanding of women’s needs.
5. Forces which dictate that good women should be ignorant about sex: In many societies the belief is that women shouldn’t take any decision on sexual activities, and most often the males dominate in taking decisions.
6. The culture of silence that surrounds sex – In many societies , women are at increased risk of HIV because lower social or economic status renders them dependent on their husband or male partner or places them in a diminished position to request that a husband or male partner be faithful or use condom, to prevent HIV transmission.
The above forces render women susceptible to HIV /AIDS. Even though it was seen early that women appear to progress to AIDS and die faster than men, it is not true. However their deaths are due to unequal access to care and treatment. Cumulative evidence indicates that women are about four times as susceptible to HIV infection as heterosexual men, based on biological / anatomical factors.
The leading cause of death in New York city for women aged 25-44 is HIV. The stigma surrounding HIV is very tragic. Even now people appear afraid to reveal their sero-status . For women the effect of AIDS stigma is usually very severe that relatives usually force women to leave their marital home after the death of a husband with a history of AIDS. One important effect of HIV/AIDS in the demographics is that, it produces a “population chimney”, with young people including women dying or becoming infertile, and so less babies, and one third of infants born to HIV positive mothers will succumb to infection. Infection is usually acquired by children of the age group 10 to 15 years who develop AIDS within 10 years. So the population of women above 20 and men above 30 decrease radically and the total population gradually decrease. HIV is highly stigmatized in India. In many countries the association between HIV and “promiscuous “ sexual behaviour has created a belief that people who are infected with HIV somehow “deserve” their fate. Paradoxically, a recent study of attitudes shows that women – who are often monogamous wives infected by their husband – are especially stigmatised. They are frequently blamed by their infected spouse, even in cases when they themselves are not infected. If a man dies of AIDS, his wife risks being thrown out of home by their in-laws.
Preventive Measures:
From the previous discussions it is clear that the only way of keeping away from HIV / AIDS is to prevent it by avoiding certain risk behaviors. Sex education delays first sex and decrease risk taking behaviour in both men and women. So young people both men and women should be given proper sex education as early as possible. It is most effective when given before the young begin their sexual lives. Well planned sex education can help reduce the risk of contracting sexually transmitted diseases, including HIV and unwanted pregnancy. So motivate men and women to talk openly about sex, sexuality, drug use and HIV/AIDS. Parents should talk to their children. Pressured to have sex, most are poorly informed about sexuality and reproduction. Parents need to talk more with their children about sex, sexuality and gender roles. Boys need to be taught that responsible sexual behaviour is a positive aspect of masculinity and both boys and girls should be offered the chance to acquire the life-skills needed to refuse sex or negotiate safer sex. AIDS prevention and care programmes are widespread but often promote broad messages that are not rooted within the context of men’s and women’s life. While abstinence and mutual fidelity are effective ways of preventing HIV infection, not everyone can, or wants to adopt these options. Even the consistent use of condoms is difficult for many men and women. So messages must reflect the realities in men’s and women’s lives. To be successful, prevention programmes must respond to realities in life. Women and men should be addressed separately and messages should be delivered to the young, the old, the rich, the poor, the urban and the rural. In some societies young women exchange sex for urgent needs for money or gifts offered to them in exchange for sex for clothing, to attend school or for food. Young girls need to be taught skills to help them reject sexual advances from men or at least to negotiate the use of condoms.
United Nations General Assembly Special Session on HIV/AIDS in June 2001 set in place a framework for national and international accountability in the struggle against the epidemic. Each government pledged to pursue a series of many benchmark targets relating to prevention, care, support and treatment, impact alleviation, and children orphaned and made vulnerable by HIV/AIDS, as part of a comprehensive AIDS response. One of the target aimed is to have by 2003, strategies that begin to address the factors that make individuals particularly vulnerable to HIV infection, including under-development, economic insecurity, poverty, lack of empowerment of women, lack of education, social exclusion, illiteracy, discrimination, lack of information and/ or commodities for self-protection, and all types of sexual exploitation of women, girls and boys. Young people and women are a priority on this front. Twenty years into the epidemic, millions of young people know little, if anything, about HIV/AIDS. According to UNICEF, over 50% of young people (aged 15– 24) in more than a dozen countries have never heard of AIDS or harbour serious misconceptions about how HIV is transmitted. Vigorous prevention efforts are needed to equip young people with the knowledge and services such as HIV/ AIDS information, condom promotion, life-skills training they need to protect themselves against the virus. Given that young people especially women are bearing the brunt of the economic transitions in the region, socio-economic programmes that can reduce the vulnerability of young men and women are also vital.
Special steps are needed to include HIV-related life-skills education in school curricula and to extend peer education to vulnerable young people who are in institutions or out of school and employment and among housewives. Much more comprehensive efforts are needed to address the complex issues related to HIV and injecting drug use among young people. Prevention is the best to avert the future cost of treating and caring the HIV affected ones. A particularly effective intervention is the prevention of mother to child transmission which is the most significant source of HIV infection in children below 10 years. This can be achieved by the primary prevention of HIV infection in parents, the prevention of unwanted pregnancies in HIV infected women and by preventing HIV transmisssion from HIV infected women to their infants. HIV infected women should have access to information, follow up clinical care and support, including family planning services and nutritional support. These can be achieved by educating and giving information and support to develop life skills to each and every girl and woman at an early age in their life that is before sexually active stage.
There is ample evidence that early, large-scale and focused prevention programmes, which include efforts directed at both those with higher-risk behaviour and the broader population, can keep infection rates lower in specific groups and reduce the risk of extensive HIV spread among the wider population. Cambodia’s prevention measures, which began in earnest in 1994– 95, saw high-risk behaviour among men fall and condom use rise consistently in the late 1990s. As a consequence, HIV prevalence among pregnant women declined from 3.2% in 1997 to 2.3% at the end of 2000, suggesting that the country is beginning to bring its epidemic under control.
In developing countries, which cannot afford antiretroviral therapy, the following are the preventive measures :
1. Access to condoms for all groups of high risk individuals.
2. Prophylaxis and treatment of infections including STD s and Tuberculosis.
3. Sex education at school and beyond.
4. Access to voluntary counselling and testing.
5. Counselling and support for pregnant women and efforts to prevent mother to child transmission.
6. Blood safety and safe injection practices.
Why women centered preventive programmes?
Compared to men, women are likely to have less formal education, less knowledge of HIV, language barriers and financial issues. Women are less likely to have a regular source of health care and are frequently unaware that they have any risk factors. Women account for a higher proportion of marginalised people with HIV, such as homeless. Also women must contend with social barrier of sexism and often dual barriers of sexism and racism. Access to treatment also is less especially to those with lower socio economic status. Women tend to have more depression. Clinical depression in HIV positive women drastically affects quality of life and greatly increases the chance of non-adherence to medications. In many societies women are at increased risk because lower socio-economic status renders them dependent upon a husband or male partner or places them in a diminished position to request that a husband or male partner be faithful or use condom, the most widely available method to prevent HIV transmission during intercourse. Many studies show that a majority of women get the infection from their sole sex partners, usually their husbands. Often women with more than one partner include those who are driven by economic necessity into sex work and they are at risk for acquisition of HIV through multiple, often unprotected, sexual exposures. So there should be an effective female controlled method so that women may protect themselves.
Future :
Ultimately the most important long term goal on HIV education and prevention involves the prevention of infection. The strategies in trial include vaccines and microbicides. Female condoms has been marketed for several years, but it is expensive for most women. Vaginal microbicides are still under research; they are extremely promising. Their advantages include non delectability including lack of smell and taste, safety and efficacy, antimicrobial properties against HIV and other STDs, and as spermicide. This may be a cream, gel, film suppository, vaginal ring or diaphragm. But all these are in the experimental field only.
Around half of the people who acquire HIV become infected before they turn 25 and typically die of the life threatening illness called AIDS before their 35th birthday. This age factor makes AIDS uniquely threatening to children. The number of AIDS orphans are gradually increasing in the world AIDS orphans means those who have lost their mother before reaching 15. Stigma is there in the provision of health care also. A majority of hospitals are reported either to turn away HIV infected patients or refuse to serve their needs. In a study of discrimination, in the health system, many health workers are of the opinion that treating patients with HIV was a waste of time and money because the patients are destined to die anyway. In this climate of irrational fear and discrimination prevention work is difficult. For prevention to be effective, culturally sensitive issues as extramarital sex and condom use must be tackled head on. Promotion of responsible reproductive health behaviour among the youth is very important. Adolescent ignorance about the sexual behaviour is compounded by the reluctance among parents and teachers to impart relevant information. Mothers expect their adolescent children, particularly daughters to remain uninformed about sex and reproduction. Sex and puberty were considered to be embarrassing and dirty subjects not to be discussed with their adolescent children. The education system is also important in sex education. Teachers also usually by and large find the topic embarrassing and try to avoid it. As a result of the reluctance on the part of parents and teachers the main source of such information is from peers and mass media. These always need not give correct information. So education becomes important in imparting knowledge on reproductive health, STDs, HIV /AIDs, moralities and principles to be adopted in life which helps to prevent transmission of HIV. If not the youth should be given information about the ways of safe sex especially the consistent use of condoms.
The objective of an AIDS control Progamme should be :
1. to bring about change in behavioural practices ( unsafe sex, sharing of needles)
2. to persuade people to take action which will safeguard them from getting infected
3. to care for the already infected without creating panic.
REFERENCES
UNAIDS Statistics 2001
UNAIDS Aids Update 1999
AIDS News.
MMWR.
Contributor
V. SUJA. Associate Professor, Department of Dermatology & Venereology and faculty, Regional Clinical Epidemiology and Resource Training Centre, Medical College, Thiruvananthapuram. Has taken M Phil in Clinical Epidemiology and M.D. in Dermatology & Venereology. Has organized various conferences. Has conducted many research projects and published papers.

